Read next
Medicine
Improving intensive care with artificial intelligence
Hospital staff usually suffer from enormous workloads and staff shortages, especially in intensive care units. This has consequences for patients, particularly when facing the prospect of multi-organ failure. In the future, Artificial Intelligence (AI) aims to enhance the application of a clinical multi-organ support system to further optimize patient treatment.
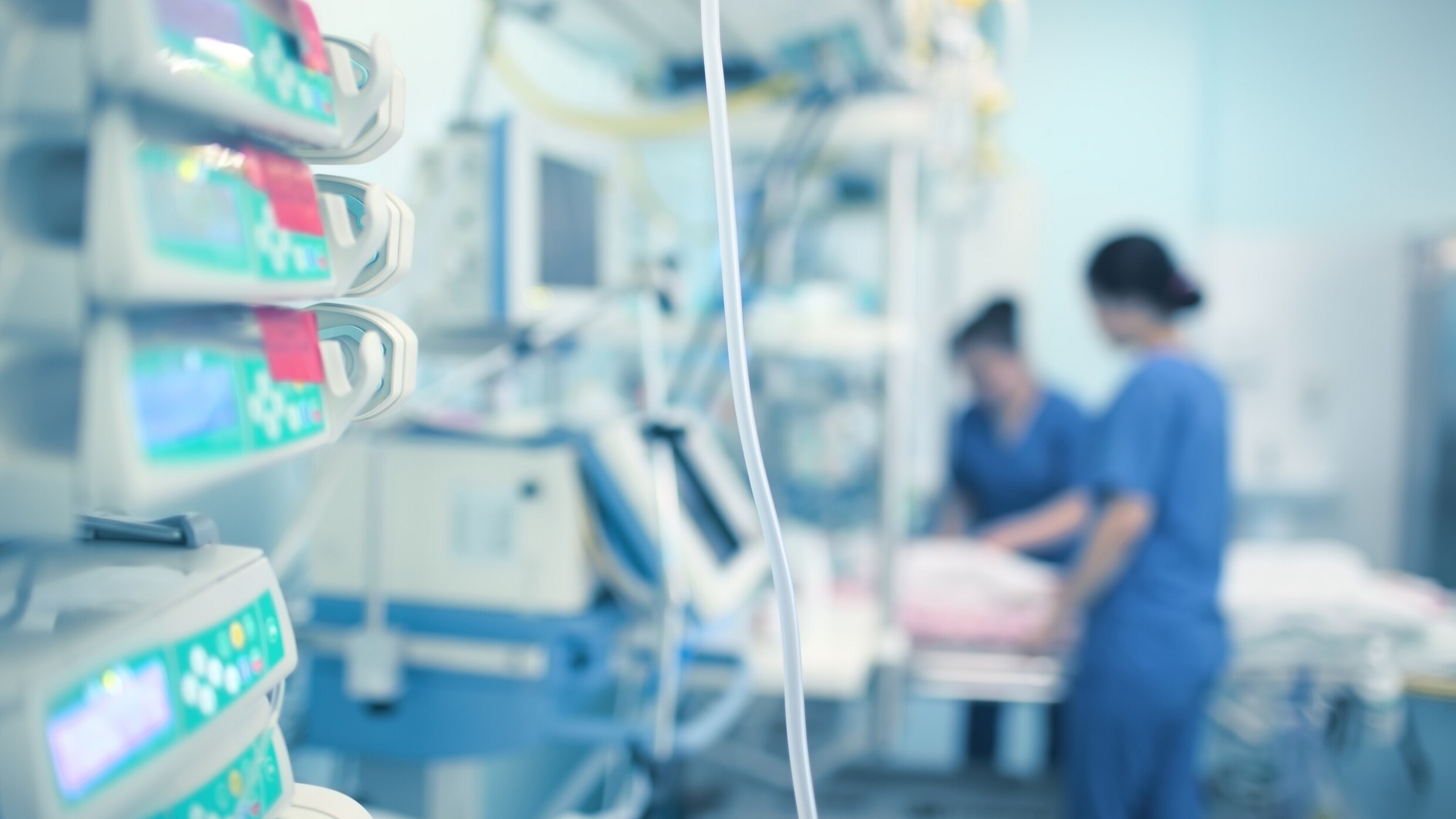

© iStock/sudok1
Working in the intensive care unit (ICU) of a hospital is a special challenge: Each moment demands delicate decision-making and rapid responses to unplanned and unpredictable events, all while bearing the weight of human lives. Added to this are shift work and a constant shortage of staff — a challenge that predates the pandemic.
In this tense situation, there is a great need for clinical decision support, the choice of treatment options, and simplifying these intricacies within the daily workings of a hospital. Notably, this would not only reduce the burden on nursing staff but also significantly improve patient care and reduce mortality.
Artificial intelligence in medicine
Find out more about Fraunhofer IKS research in the field of artificial intelligence in medicine on our website:
Mortality in multi-organ failure
Approximately 60% of deaths in ICUs are due to multi-organ failure— around 500,000 cases annually across Western Europe and the United States. Mortality increases in particular when the liver, lungs, and kidneys are compromised. Until now, in such scenarios, a separate device was connected for each failing organ. However, this approach can worsen the patient's condition, as it fails to account for organ interactions leading to an increased risk of complications. In addition, the presence of multiple devices hampers caregivers direct access to the patient.
Simplifying multi-organ support system using AI
ADVITOS GmbH, a partner of the Fraunhofer Institute for Cognitive Systems IKS, has developed and approved the ADVOS multi, a multi-organ support system for systemic treatment of multi-organ failure. ADVOS multi provides support for the main detoxification organs, the liver, lung, and kidney, as well as control over blood pH management, all within a single device.
The treatment of multi-organ failure is intricate, demanding a high level of experience from both the clinical users and the service personnel. This is where a joint project between ADVITOS and Fraunhofer IKS comes in: AI is used to support the device users in making optimal treatment decisions, thus enabling refined and individualized therapy.
Learn more!
You want to learn more about the research of Fraunhofer IKS on AI in medicine? Then please feel free to contact our Business Development for a personal conversation at business.development@iks.fraunhofer.de
To achieve this, "Big Data" pools are initially generated through laboratory experiments and later in clinical settings. These pools are then interconnected and from their correlations novel clinical recommendations and predictions can be derived. This will then be used to create a decision support system as part of the project, which is set to be validated and further refined during clinical deployment. In this way, the immense complexity of multi-organ failure will be addressed systematically and targeted, moving away from treating failing organ systems in isolation. This will reduce the workload of intensive care nursing staff in the future and ensure optimal care for patients.
The project is awaiting funding from the German Federal Ministry of Education and Research as part of the call for "Medical Technology Solutions for Digital Healthcare".


